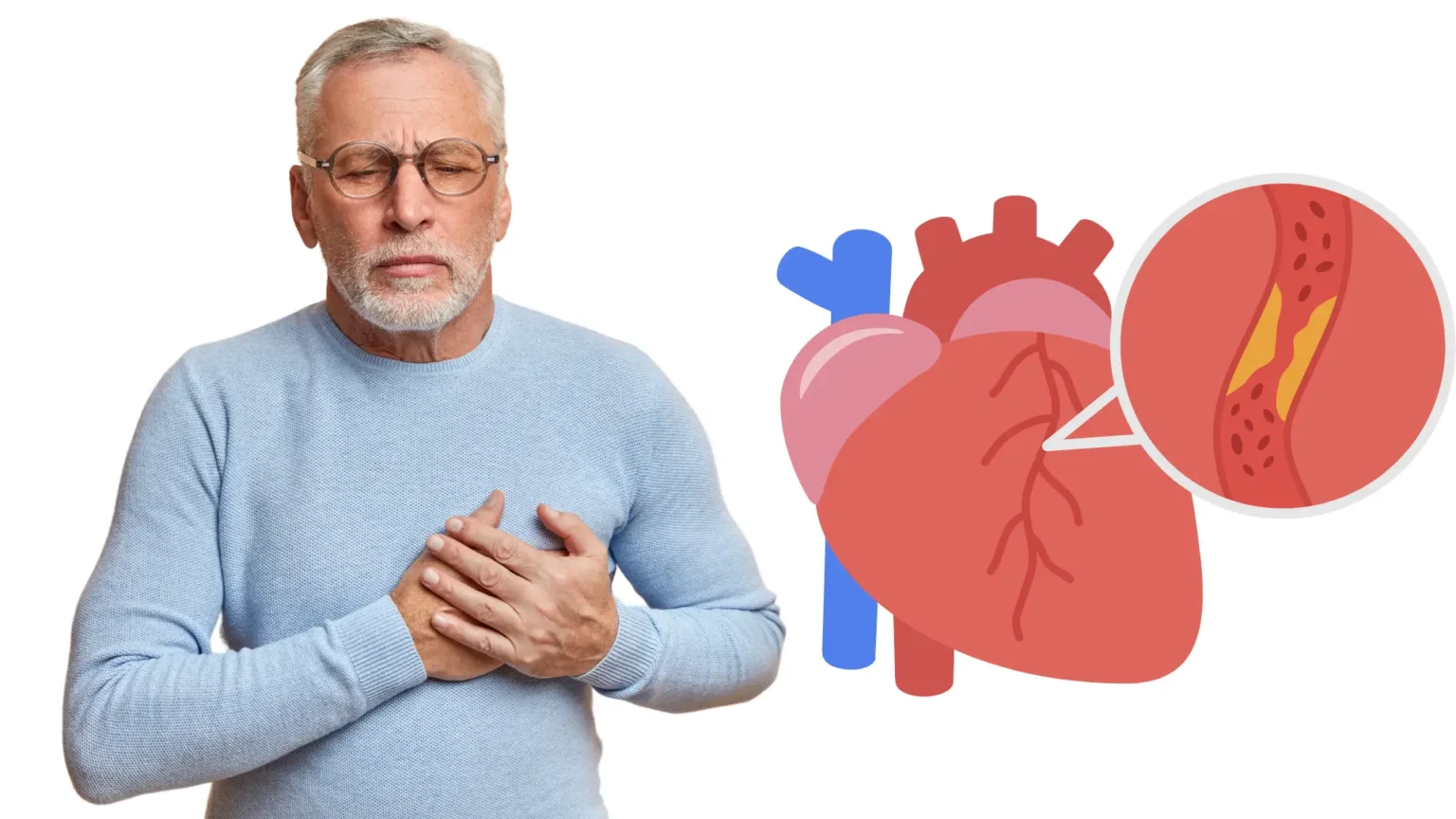
Chronic occlusion occurs when an artery becomes severely narrowed or completely blocked over time, limiting the amount of blood that can reach certain tissues. Because the blockage develops gradually, treatment strategies must address both the current symptoms and the underlying causes of vascular disease.
Modern cardiology offers several effective options—from medication to advanced interventions—designed to restore circulation and protect future heart health. At Liv Hospital, specialists evaluate each patient individually to determine the safest and most effective approach. You can also review the official page on CARDIOLOGY Treatment and Rehabilitation to understand how treatment plans are structured.
Personalized Treatment Planning
No two patients experience chronic occlusion in the same way. Doctors consider multiple factors before recommending therapy, including:
- the location of the blockage
- severity of symptoms
- overall cardiovascular health
- presence of other medical conditions
- age and lifestyle factors
The primary goals of treatment are to restore blood flow, reduce symptoms, prevent complications, and improve quality of life.
Medication as the First Line of Treatment
For many patients, medication plays an essential role in controlling symptoms and preventing the condition from worsening.
Antiplatelet therapy
Antiplatelet medications reduce the risk of blood clots forming on existing plaque. By preventing platelets from sticking together, these drugs help maintain smoother blood flow through narrowed arteries.
Cholesterol management
Lowering cholesterol is a major part of treatment. Statins and other lipid-lowering medications help reduce plaque buildup in the arteries and stabilize existing deposits so they are less likely to rupture.
Blood pressure control
Managing blood pressure reduces the strain on artery walls and helps prevent further vascular damage. Medications such as ACE inhibitors or beta-blockers may be recommended depending on the patient’s condition.
These medications are often used together as part of a long-term cardiovascular protection strategy.
Minimally Invasive Procedures to Restore Blood Flow
When medications alone cannot relieve symptoms, doctors may recommend interventional procedures to open the blocked artery.
Angioplasty
Angioplasty is a catheter-based technique used to widen narrowed arteries. During the procedure:
- A thin catheter is inserted through a blood vessel.
- A small balloon at the tip is inflated to widen the blocked artery.
- Blood flow improves once the artery expands.
Stent placement
In many cases, a stent is placed during angioplasty. A stent is a small mesh tube that keeps the artery open and prevents it from collapsing again.
Advancements in cardiology technology have made these procedures highly effective, with many patients experiencing significant symptom relief shortly after treatment.
Surgical Treatment for Complex Occlusions
Some blockages are too long or heavily calcified for catheter-based procedures. In these situations, surgery may be recommended.
Coronary artery bypass surgery
This procedure creates a new route for blood to travel around the blocked artery. Surgeons use a healthy blood vessel from another part of the body to bypass the occlusion.
Peripheral artery bypass
For blockages affecting the legs, a similar technique is used to redirect blood flow around the blocked artery.
Although surgery involves a longer recovery period, it can provide long-lasting improvement in circulation and reduce symptoms significantly.
The Role of Cardiac and Vascular Rehabilitation
Treatment does not end with medication or procedures. Rehabilitation programs are designed to help patients regain strength and prevent further cardiovascular problems.
Rehabilitation programs typically include:
- medically supervised exercise training
- guidance on safe physical activity levels
- nutritional counseling for heart-healthy diets
- education about managing blood pressure and cholesterol
- strategies for stress reduction
Structured rehabilitation can improve endurance, circulation, and confidence during recovery.
Lifestyle Adjustments After Treatment
Successful recovery also depends on lifestyle changes that support vascular health. Doctors often recommend:
- quitting smoking
- maintaining a healthy weight
- following a balanced diet rich in fruits, vegetables, and whole grains
- engaging in regular moderate physical activity
- managing diabetes and blood pressure carefully
These steps help prevent the formation of new blockages and protect long-term heart function.
Long-Term Monitoring and Follow-Up
Patients treated for chronic occlusion usually require ongoing monitoring to ensure the artery remains open and circulation remains stable. Follow-up visits may include imaging tests, stress tests, or adjustments to medications.
Regular checkups help detect potential issues early and allow doctors to refine treatment plans when necessary.
Supporting Recovery Through Healthy Living
Medical treatment and rehabilitation form the foundation of recovery, but long-term cardiovascular health also depends on daily habits and overall wellness. Maintaining balanced routines, stress management, and healthy lifestyle choices can complement medical care and support ongoing recovery. For additional lifestyle inspiration and wellness guidance, you can explore helpful resources at live and feel.